- Phase two of Economist Impact’s Health Inclusivity Index, supported by
Haleon , measures experience of health inclusion across 42,000 people in 40 countries - Health inclusivity scores fall worldwide with addition of lived experience data, exposing glaring policy-practice gap in wealthy countries
- 66% of survey respondents experience barriers to health inclusion, with the most vulnerable worst affected
- Index reveals stark generational divide with Gen Z and Millennials experiencing greater barriers to access and higher levels of discrimination
This year’s study – which measures the extent and experience of health inclusion across 40 countries and 42,000 people – revealed that 66% of those surveyed face at least one barrier in accessing healthcare services. Lack of available appointments; inconvenient hours; distance and cost of travel; and lack of trust in healthcare services were the most widely reported barriers. Alarmingly, the Index also revealed that one in five people worldwide (20%) lack access to mental health services in their community, while 17% lack access to sexual health services.
The study suggests that younger generations face particular issues, with almost half of Gen Z (45%) stating their quality of care has been compromised as a result of their age, health status, or other personal factors, compared with 19% of Baby Boomers. Almost a third of Gen Z (28%) and Millennials (32%) report that their pain or health conditions are not taken seriously by healthcare professionals. While almost a quarter of Gen Z (21%) and Millennials (22%) report they’ve been completely denied access to healthcare, compared with just 8% of Baby Boomers.
Besides appointment hours and availability, together with distance and cost to travel, Gen Z are the most likely to cite lack of trust in healthcare providers and fear of discrimination as major obstacles when seeking healthcare services. 44% of Gen Z also cited social media as a trusted source of health information and advice – the highest proportion amongst all generations surveyed.
The most vulnerable populations, namely people from marginalised groups and those with chronic health conditions, also report being denied access to healthcare (26%). Discrimination is a key barrier, with more than a quarter (27%) of those from marginalised groups and people with chronic health conditions experiencing this when interacting with healthcare providers.
The first phase of the Index, launched in 2022, examined the presence, coverage and effectiveness of inclusive healthcare systems, policies and programmes. The research methodology for 2023’s phase two study has been enhanced to include an assessment of people’s experience of these inputs – by capturing insights from 42,000 people to understand their experiences of health inclusion or exclusion.
With the addition of this lived experience data, health inclusivity scores have deteriorated under phase two of the Index across 85% of the countries surveyed. For example, the UK’s score fell by 13%, falling from first to third place, behind
The declining scores year-on-year expose a policy-practice gap between governments’ ambitions of delivering inclusive health policies and systems and people’s real-life experience of them. High income countries display the largest gaps, with an average 18-point difference between their scores on inclusive health policies and people’s real-life experience, with
In common with last year’s findings, phase two of the Index concludes that empowering people and communities to have greater agency over their own health is a key driver of inclusion. Low-and-middle income countries outperform wealthier countries in this area due to their focus on community-based services, self-care and health literacy programmes. For example, 73% of people in low-and-middle income countries have been given advice or information on managing their health at home, compared with 65% for high-income countries.
Consequently, low-middle income countries display an average policy-practice gap of just 3-points and are more effective at ensuring inclusion for marginalised groups, those with chronic health conditions and Gen Z. The fact that countries with less developed infrastructure, lower spending and fewer resources are more effective in delivering population-level health inclusivity in practice is a rich source of learning for both high-and lower-income countries.
As a global leader in consumer health,
Under phase two of the Health Inclusivity Index,
| Media Contacts: | |
| Haleon Media Contact: Gemma Thomas gemma.x.thomas@haleon.com +44 (0) 7721376006 | Economist Impact Media Contact: hollydonahue@economist.com |
Notes to Editors:
About
Haleon’s social impact goal is to empower millions of people a year to be more included in opportunities for better everyday health – with the company aiming to reach 50 million people a year by 2025. During 2022, we empowered more than 22.4 million people.
We have identified three key barriers to health inclusivity that
• health literacy;
• healthcare accessibility; and
• bias & prejudice
Examples of Haleon’s efforts to break down barriers to health inclusivity include:
Health Literacy:
Our Caltrate calcium supplement brand in
Healthcare Accessibility:
To help make our brands more accessible, we have collaborated with Microsoft on expanding the functionality of their Seeing AI app for
Bias and Prejudice:
About
For more information, please visit www.haleon.com
About Economist Impact
Economist Impact combines the rigour of a think-tank with the creativity of a media brand to engage a globally influential audience. We believe that evidence-based insights can open debate, broaden perspectives and catalyse progress. The services offered by Economist Impact previously existed within
A photo accompanying this announcement is available at https://www.globenewswire.com/NewsRoom/AttachmentNg/a24060d5-eb9b-4fa1-8cbf-e5427cfaaa24

![]()
Year 2 Health Inclusivity Index Scores
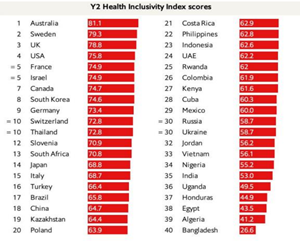
Under phase two of the Health Inclusivity Index, Australia achieves the highest score, followed by Sweden , UK , USA , France , Israel , Canada , South Korea , Germany , Switzerland and Thailand
2023 GlobeNewswire, Inc., source




